by Mark van Gils (VTT)
Decision making for complex diseases requires efficient consideration of information from a large variety of very different data sources. We developed a machine-learning based decision support system for dementia diagnosis and evaluated it within four hospitals in Europe.
Clinical decision making is often fraught with difficulties related to extracting the right information from huge amounts of diverse data. Complex diseases are diseases in which diagnosis making is difficult. This may be, for instance, because symptoms are non-specific (different diseases cause similar symptoms), or there is high variability between individuals in how the disease manifests itself, or there is no objective gold standard regarding diagnosis.
An example of a complex disease is dementia. It is important to detect dementia as early as possible, before late-stage symptoms, such as severe memory problems become obvious, and there is no longer any room to improve quality of life. It is also important to discern between the different forms of dementia (differential diagnosis), in order to provide appropriate interventions. Different forms of dementia include Alzheimer’s disease (the most prominent form of dementia), vascular dementia, dementia with Lewy bodies, and frontotemporal dementia. To confuse the matter, healthy subjects may present with memory complaints similar to those of dementia patients.
Clinicians need to combine a wide range of data sources upon which to base decisions. This information may range from imaging data (MRI, CT, and sometimes PET scans) to blood tests, genetic information, neurospsychological tests, text data from interviews and different -omics data. Additionally, data such as background information, as well as financial and feasibility constraints, need to be considered when deciding on appropriate interventions for an individual. The decision making also has a subjective component, based on personal experience. This complexity easily leads to less-than-optimal decision making, even if profound clinical expertise is available.
In addition to the complexity and diversity of the data, there are issues related to quality and availability. Not all data is available from all patients (different clinics have different resources, equipment and protocols), data quality may be less than optimal and the data may be in different formats and have different properties related to equipment and measurement environments. Clinical decision support systems (CDSS) based on principles of data-driven medicine potentially make the process more quantitative and objective. They thus may help to provide more confidence in the decision making for complex diseases.
In the EU-funded project VPH-DARE@IT [L1] a patient care platform was developed, and subsequently validated in the project PredictND [L2], that implements a CDSS integrating biomarkers from medical images, neuropsychological tests and other measurements. VTT and Combinostics Ltd. took care of the technical development, and clinical partners provided the needs and data for development and validation. The system helps form a multi-variate integrated and easily understandable view of a patient’s status based on machine learning and data visualisation methods. It uses an approach where large multi-centre databases of previously diagnosed patients are used to build mathematical models of several dementing diseases, such as Alzheimer’s disease, frontotemporal dementia, vascular dementia and dementia with Lewy bodies. When a new patient arrives at a clinic, measurements are done, that are then compared with the disease models. The software architecture enables access to heterogeneous patient data from a large variety of data sources in different hospital settings.
The system’s analysis functionality has two main components: automatic segmentation and quantification of brain images and a supervised machine learning method for assessing and visualising the multi-variate state of patient with respect to the investigated diseases. First, fully automated image processing methods derive volumetric measures from brain MR images. Second, the quantified imaging data are combined with all other available data, including demographic information, neu-ropsychological test results, blood test analysis, CSF (cerebrospinal fluid) analysis and the patient’s genetic profile. A machine-learning paradigm, the Disease State Fingerprint [1], takes all patient data and compares it to previously diagnosed patients, providing an index of similarity with each disease profile. Moreover, it provides an interactive visual representation of the multi-variate patient state, allowing the clinician to understand which variables contribute to the decision suggestion, and how each contributes (Figure 1). It can show the overall “disease probability”, but also allows the user to zoom in to the distributions at detailed feature level to show, for instance, how the current patient’s measurements compare to the different disease-related distributions in the database. The methods work with interval, ordinal as well as nominal data, and have been designed from the ground up to handle issues that are important in clinical decision making. These include dealing with missing data (“incomplete input vectors”) and the demand for explainabality of classification results (“non black-box functioning”).
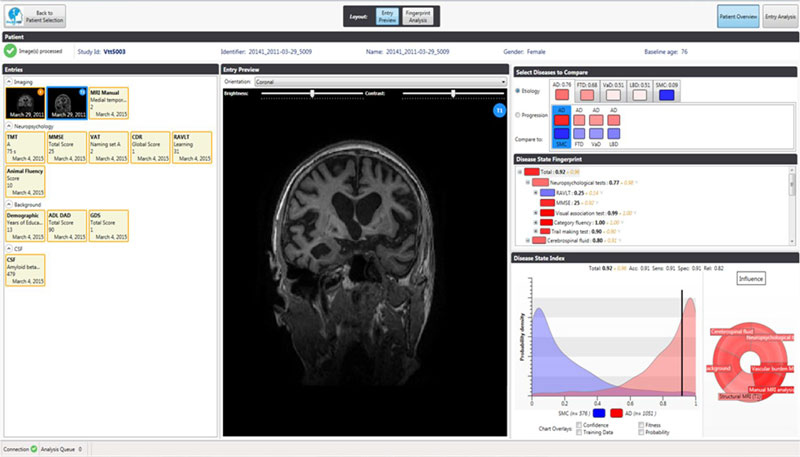
Figure 1: A screenshot of the decision support tool. On the left-hand side the different information sources are shown, including, in this example, MRI imaging data, neuropsychological test results, background information and cerebrospinal fluid (CSF) data. The middle panel shows the image analysis view which allows for automatic segmentation, quantification and visualisation of relevant parts of the brain. The right hand panel shows the multi-variate decision support functionality. At the top, the various forms of dementia that can be considered are shown, below is a “disease state fingerprint” indicating visually and quantitatively to which disease group this patient most likely belongs, together with the relative importance of the different variables. Finally, the raw data distributions of separate variables can be examined in the bottom right panel.
The methods have been shown, using cross-validation, to reach a classification accuracy of 82 % when discriminating patients between five different memory problems [2]. The clinical decision support tool using these methods was validated with 800 prospective patients, to examine how it performs, both quantitatively and from a usability perspective, with real users at four memory clinics across Europe (Finland, Denmark, The Netherlands and Italy) [3]. The results of this study showed that addition of the CDSS to the existing clinical process affected the diagnosis and increased clinicians’ confidence in the diagnosis indicating that CDSSs could aid clinicians in the differential diagnosis of dementia.
This work has been co-funded by the EC under Grant Agreements 601055 (VPH-DARE@IT) and 611005 (PredictND).
Links:
[L1] http://www.vph-dare.eu/
[L2] https://www.predictnd.eu/
References:
[1]: J. Mattila, J. Koikkalainen et al.: “Disease State Fingerprint for Evaluating the State of Alzheimer’s Disease in Patients”, J Alzheimers Dis, vol 27, pp. 163-176, 2011.
[2]: A. Tolonen, H. Rhodius-Meester et al.: “Data-Driven Differential Diagnosis of Dementia Using Multiclass Disease State Index Classifier”, Frontiers in Aging Neuroscience, vol. 10, , pp. 111, 2018.
[3] M. Bruun, Marie; K.S. Frederiksen et al.: “Impact of a Clinical Decision Support Tool on Dementia Diagnostics in Memory Clinics: The PredictND Validation Study”, Current Alzheimer Research, vol. 16, pp. 91-101, 2019.
Please contact:
Mark van Gils
VTT Technical Research Centre of Finland Ltd., Finland
tel. +358 20 722 342











