by Sara Gestrelius and Martin Aronsson, SICS Swedish ICT
When a woman is diagnosed with breast cancer she is drawn into a network of examinations, tests and treatments with interdependencies in several steps. Because the prognosis for recovery is tied to how quickly she gets help, it is important to reduce the time from the first doctor’s appointment to the start of treatment.
In early 2013 the health authorities of Region Östergötland in Sweden were investigating why the time between the first doctor’s appointment and the start of treatment was longer than the goal of 28 days for breast cancer patients at the hospital in Linköping. To help answer their question, researchers from SICS Swedish ICT were tasked with proposing and testing operational research methods that could elucidate how the different process steps contributed to the overall lead time. The methods proposed should also allow for different process changes to be investigated.
The pilot study began with an investigation step where the researchers learned about all parts of the care process. This included interviews with doctors and administrative staff, and also analysis of data that the department had gathered over the years. The initial analysis resulted in some important insights about the process, e.g. that the patient inflow varied depending on the time of the year, and that the process had a number of discrete steps that negatively affect the lead time. In fact, based on the initial analysis it could be proven that the goal lead time of 28 days or less was impossible to live up to for many patients, given the current process and methods. Patients arriving on certain week-days were out of sync with the discrete process-steps, which resulted in long lead-times.
The discrete steps are often a consequence of doctors having certain days allocated to certain tasks, or operating rooms only being available on certain days. This is because operating rooms are shared among departments, and set-up times prevent doctors from performing all tasks every day. For example, the doctors do not have time to hold multidisciplinary conferences every day. The focus on high resource efficiency negatively affected the patient flow.
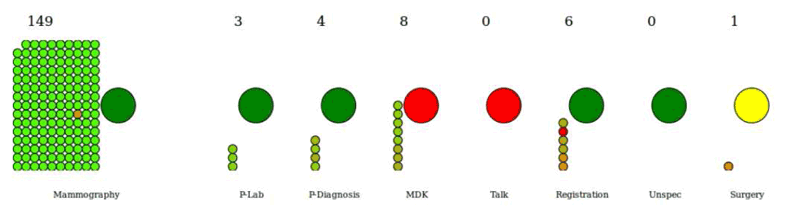
Figure 1: Example of a simulation of a care process. The small circles are patients, and the colour represents time since their first doctor’s appointment. The large circles are process-steps that are open (green), open but working at full capacity (yellow) or closed (red).
Based on the understanding acquired in the investigation step we constructed a discrete event simulation. The arrival process was modelled as an inhomogeneous Poisson process based on the historic data, and the basic rules of the simulation model were reviewed by the interviewed staff. The purpose of the simulation was to investigate whether there was potential for shorter lead times, and if so, where to invest in resources. First of all the lead times from the simulated standard process and the historic data were compared, and the discrepancies were discussed with the hospital staff. Then different proposed process changes were tested in the simulation to provide insights that were otherwise difficult to gain. For instance, the simulation could detect when increasing resources in a particular process step did not result in time gains because the patient still had to wait for other parts of the process. The simulation model was also used to estimate how congested the different process steps were. Being able to explore the process, and predict and quantify in advance how changes affect the lead time and the load curve, stimulated great interest among the hospital staff.
In addition, the hospital identified a few departments with resources that were likely to benefit from optimizing planning support systems. Operating rooms, as well as other shared resources such as pathology analysis competence, are interesting subjects for optimization and planning as they deal with demands from many patient streams and categories.
Shorter lead times are closely linked to the question of good planning. Of course you always have to be particularly considerate when working with people. Perhaps the patient needs a few extra days, for instance, to take in the news that she has cancer before she is ready to go into surgery. Nevertheless, SICS believes that a more industrial approach to the planning process would benefit everybody involved. Apart from using simulation there are other operational research techniques that are apt for healthcare systems, such as optimization of schedules [1].
The SICS researchers involved with the project consider healthcare a perfect candidate for their planning methods. They think better decision support tools would enable a care that is more adapted and coordinated, both for the patient and for the health professionals.
Link:
http://www.sics.se/projects/flecs-flow-efficiency-in-cancer-treatment
Reference:
[1] M. Persson: “On the Improvement of Healthcare Management Using Simulation and Optimisation” Blekinge Institute of Technology, Karlskrona, doctoral thesis, 2010.
Please contact:
Sara Gestrelius, Martin Aronsson
SICS Swedish ICT











